The pulse is a vital sign of life. Medicine past and present has measured the rhythmic pulsation that can be felt at various points on the body for signs of illness, love and stress. From birth to death, your pulse confirms that you’re alive. You can’t live without a pulse – or can you?
Alongside body temperature and breathing, the pulse is a vital sign of life – a measure of the body’s most basic functions that are routinely checked by medical practitioners. When a baby is born the pulse or heart rate is one of the first things to be checked as part of the Apgar score (appearance, pulse, grimace, activity, respiration), a quick method used to determine how well the baby is doing.

The examination of the pulse has always been an integral part of Ayurvedic medicine. The Indian physician and philosopher Kanada (c. 600 BCE) wrote about using the pulse to diagnose illness. In the Ayurvedic system, diseases were thought to arise from the ‘eccentricity’ of the three humours, báyu (air), pitta (bile) and kaph (phlegm), which resulted in variations in the pulse. Kanada likened different rhythms to the movement of animals, such as serpents and frogs, and used them to assess the severity of health conditions.
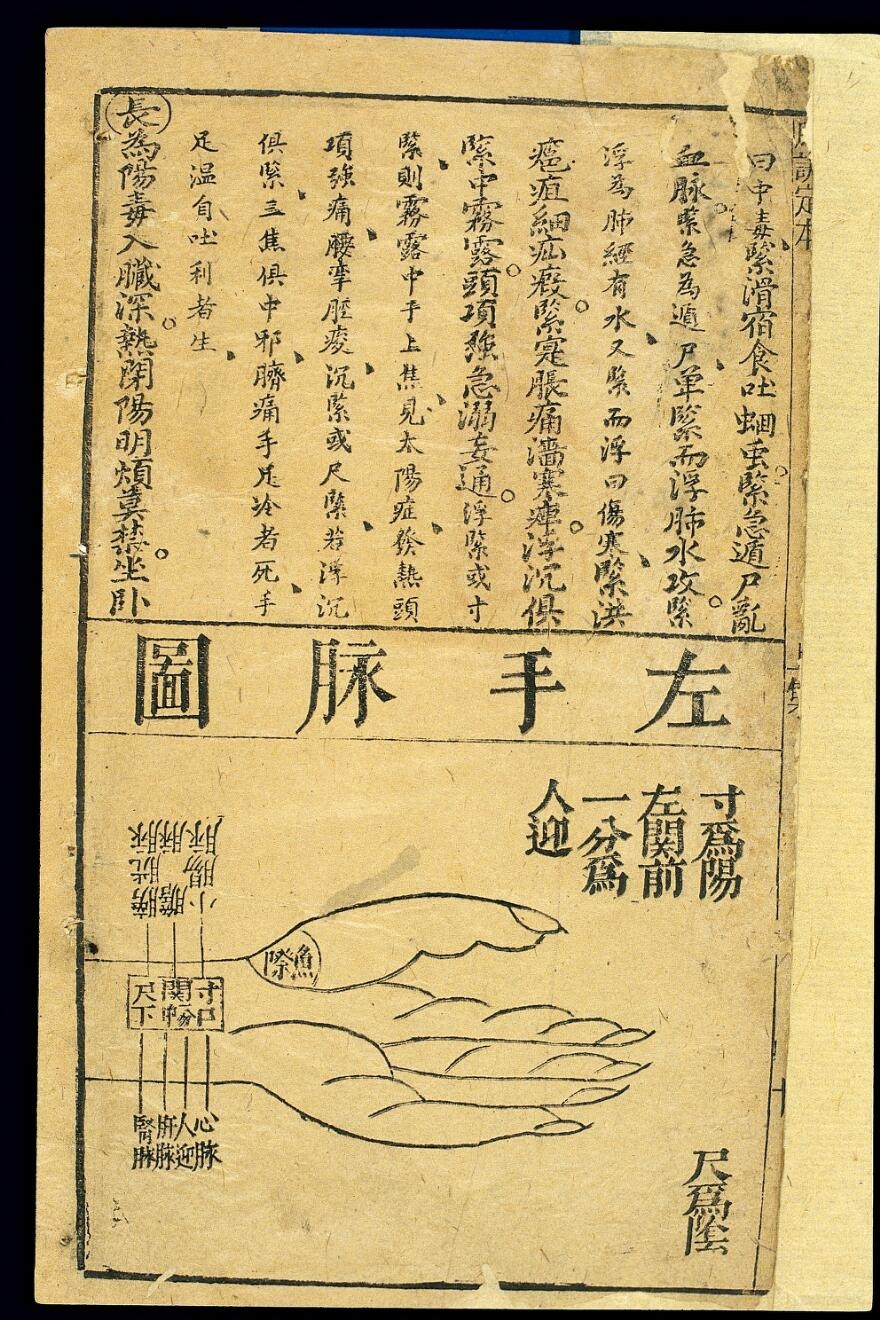
In traditional Chinese medicine, pulse diagnosis was developed to a sophisticated level. This illustration demonstrates how the pulse was measured in three locations on the left wrist. Each location is associated with different organs, for example, the cunkou pulse is associated with the heart and small intestine, the guanzhong with the liver and gall bladder, and the chixia with the kidney and bladder.

The Persian physician and scholar Ibn Sina (980–1037 CE) studied the characteristics of the pulse in great detail, noting the differences in the regularity of rhythms, the size of the arterial dilations and temperature at the time the pulse was taken. He not only recognised the pulse as a measure of physical health, but he also linked it to the emotions, age and sex. Among his diagnoses was one for lovesickness.
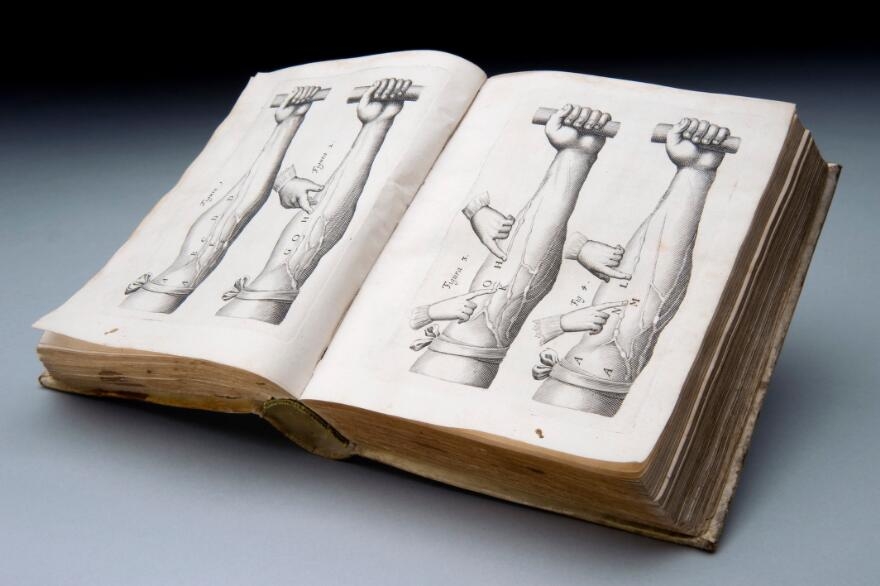
In the 17th century the English physician William Harvey confirmed that blood circulated around the body, pumped by the heart. His work established the connection between the pulse and the contraction of the heart. It defined the pulse as the rate at which the heart beats (usually measured in beats per minute). An understanding of the blood-circulation system gave rise to another vital measure of health: blood pressure. This is a measure of the force that your heart uses to pump blood around your body. The pulse (heart rate) and blood pressure together are still used as important diagnostic indicators.
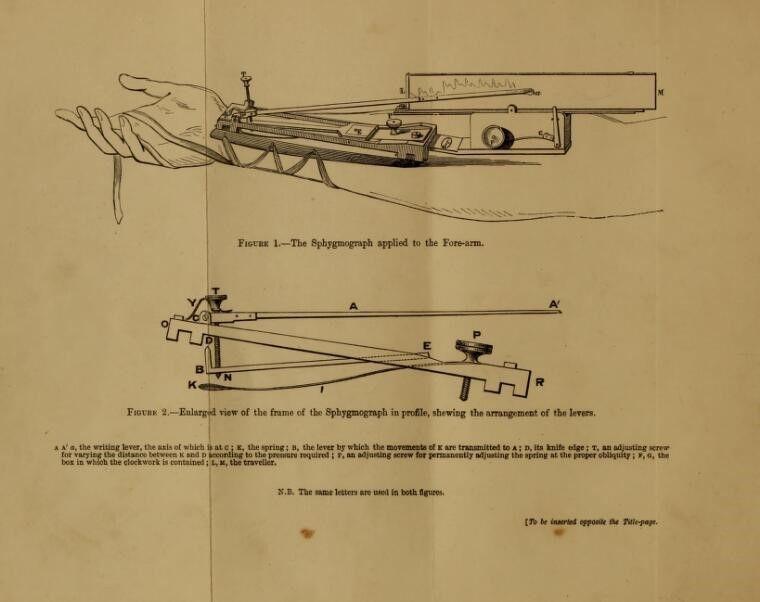
The French physiologist Étienne-Jules Marey (1830–1904) developed the sphygmograph, to be placed above the radial artery in order to magnify and record the pulse on paper with an attached pen. Now the pulse could be seen, recorded and compared, rather than relying on the subjective feel of the physician’s fingertips. The sphygmograph was a forerunner of the sphygmomanometer blood-pressure monitor familiar to many of us in the form of an inflatable cuff attached to a pressure-measuring device.
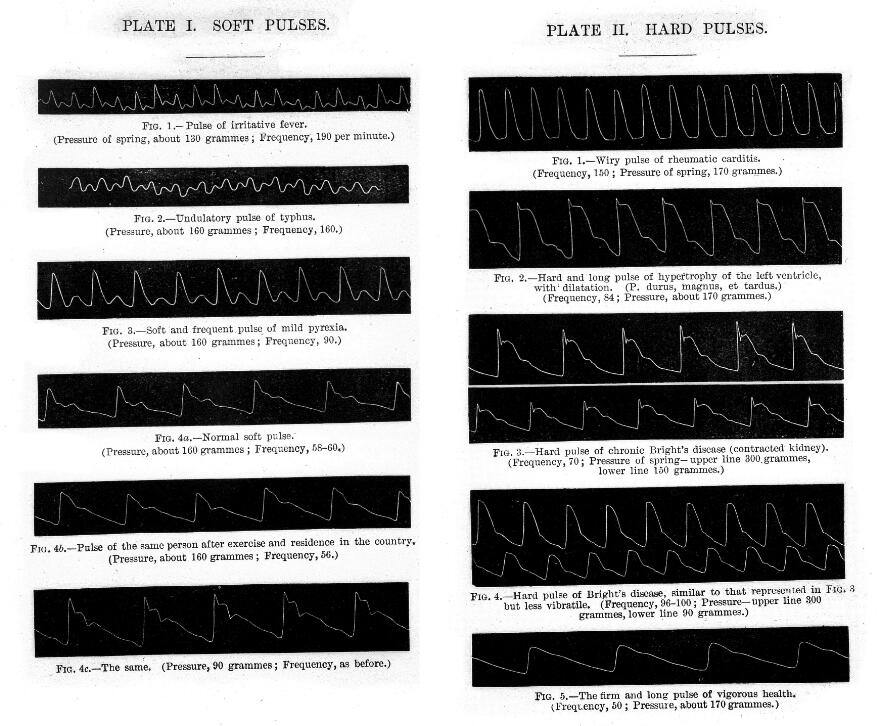
The trace generated by the sphygmograph was a measure of the rise and fall of the pulse as well as blood pressure. Using sphygmograph traces to diagnose illness became a standard technique in late-19th-century medicine. Sphygmographs were superseded by ECG devices (electrocardiography), which measure the electrical activity of the heart through electrodes placed on the skin.

Up to the early 20th century blood pressure and pulse devices had been used to gather information for medical purposes. In 1917 psychologists William and Elizabeth Marston began to explore an alternative use for these devices, stemming from Elizabeth’s suggestion that “when she got mad or excited, her blood pressure seemed to climb”. The Marstons’ work laid some of the foundations for the polygraph or lie detector. Although the results are inadmissible in criminal courts in the UK, polygraphs are still used during the investigative process.

The same phenomenon that gave rise to the polygraph also accounts for another phenomenon: white coat syndrome. It’s well known among health practitioners that patients can present with higher blood-pressure readings when they are at the doctor’s surgery or hospital than when taken at home. This may well be due to the temporary stress or worry of being in a medical setting.
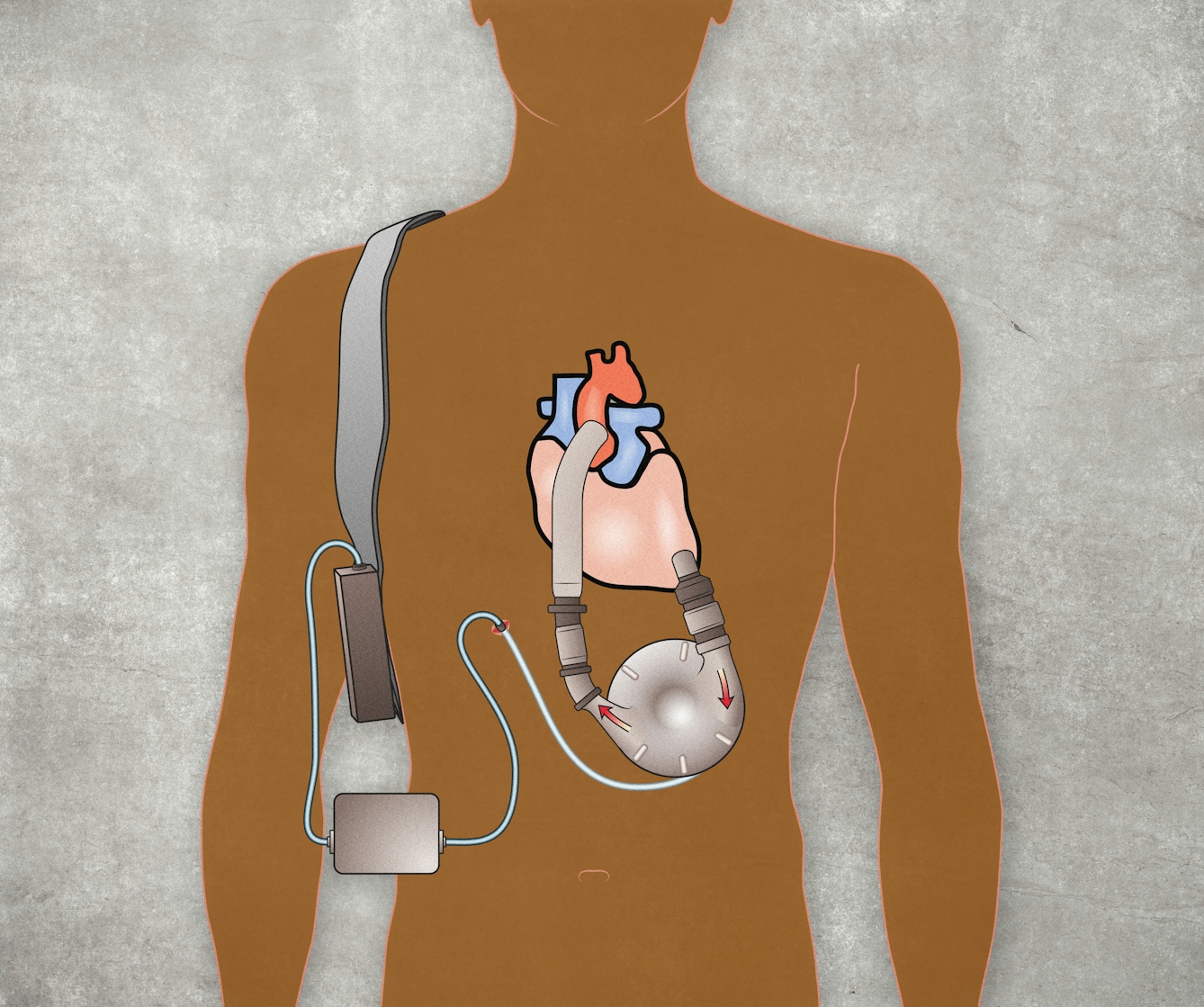
The pulse and blood pressure are key to measuring the health of your heart, and variations in either can be signs of heart disease. While heart transplants offer the best hope for those with acute heart disease, a piece of equipment called a ventricular assist device (VAD) can act as an artificial heart. It works by taking over from the heart muscle to circulate blood around the body through an external pump. The VAD transforms lives, giving people the vigour and energy that they had lost. One version of the VAD generates a continuous flow of blood, rather than a regular pulsation. For the thousands of people who use this model, losing your pulse is a sign that you’ve got your life back.
About the author
Anjuli Sharma
Anjuli is a graduate trainee at Wellcome. Prior to joining Wellcome, she studied Pharmacology and Physiology at King’s College London.