Today’s smartwatch health apps follow hundreds of years of people trying to measure and record health information. Ross MacFarlane shows how tracking health (and ill health), whether by the state or by the self, has a long and rich history, encompassing plagues, wars and consumerism.

Surveying a population is by no means a modern invention. Early censuses were used to collect details for tax purposes or to show who could be mobilised for war, but who could work or fight, and how, revealed demographic and health information to governors too. This image depicts the biblical story of Joseph and Mary registering for the census in Bethlehem, the home of Joseph’s ancestors. They had to travel there due to the rules of the Roman census, and Bethlehem thus became the site of Jesus’s birth.

As well as rulers taking measurements to know how their states worked, even hundreds of years ago people took measurements to know how their bodies worked. Santorio Santorio (1561–1636) was an Italian physician who could perhaps be described as the first health ‘self-tracker’. His method included – as pictured here – sitting in a balance to calculate how his weight changed over time after eating – and then excreting – food and drink.This shows the beginning of weight measurement becoming a significant factor in medicine, and the notion of self-measurement too.

Bodies stopping working, due to dropping dead, was the most pressing concern for both individuals and the state to measure and try to prevent. After the Black Death of the 14th century, mortality was recorded in more formal ways during plague epidemics. Then, from the 16th century, Bills of Mortality gave information about the births, deaths, and causes of death in London parishes. John Graunt (1620–74) applied statistical models to the Bills to suggest comparative birth rates, mortality rates and disease spread. His book ‘Natural and Political Observations Made upon the Bills of Mortality‘ (1662) is one of the earliest works of demography, though he voiced concerns about the accuracy of the Bill data.

Since the pandemic, we have become used to seeing graphs of death rates rising as disease spreads, but access to such numbers was once a new and disturbing phenomenon. This letter from 19 June 1665 offers a rare insight into an early reader’s experience of seeing deaths rising on the Bills week by week. John Moore (1620–1702) writes to his cousin, “The plague increaseth much and spreads it selfe very strangely in the Citty and suburbs. 17 dyed one week 43 next and last weeke 112 of the plague and of all diseases 558 (last weeke) and much feared this weeks bill will farr exceed the last.”

Mortality statistics were more useful to governments if they were clear about why someone had died. From 1837, people had to report deaths to registrars, but a medic did not have to certify the death and the cause of death was not always systematically recorded. To help clarify causes of death, in 1839 William Farr devised the first system of disease classification, or nosology, for the General Register Office. The image here is from the GRO’s 1843 ‘Regulations and a statistical nosology: comprising the causes of death, classified and alphabetically arranged’.

Victorian Britain increasingly relied on surveys and statistics to understand people and establish norms. This data was used to prevent deaths and keep people productive, particularly after the cholera epidemics of the 1830s and 1840s drew attention to links between poverty, ill health and growing urbanisation. Medical Officers of Health were hired to enforce legislation, monitor rules, and accumulate data on public health, such as rates of infectious disease. Over time, they grew more powerful, and their work reached further and further into the homes and lives of local people.

Medical technologies enabled yet more data to be collected by Medical Officers of Health and by individual people. One example is thermometers – which became more readily available by the mid-19th century. This cartoon from ‘Punch’ magazine mocks the ignorance of people wanting to use new technologies without understanding them: the pharmacist thinks the customer wants to purchase a thermometer (when it seems the customer’s doctor has actually suggested a thermostat to regulate the temperature of her home). A rather paltry 19th-century joke, but it shows how many different types of data, environmental and biological, could now be collected to monitor health.

Bodies and environments came under greater scrutiny during wartime as well as epidemics. After the Boer War (1899–1902), British authorities were concerned about why the British Army had performed so poorly against the Boer forces. The Report of the Inter-Departmental Committee on Physical Deterioration focused on the apparent physical deterioration of the young working-class men who had volunteered to fight. The report emboldened advocates of eugenics to push for their ideas on how to “improve the stock” of British fighting men. It recommended more physical education in British schools and improved housing for working-class families.
To make fit soldiers and workers, governments increasingly focused on their early lives, and creating fit infants and children. The headline from this French inter-war poster can be translated as “Baby’s growth must be constantly monitored”. This instruction for parents from the National Committee for Children – with its calls for constant watching, surveillance and measurement – speaks to the broad themes of French philosopher and historian of ideas Michel Foucault (1926–84), who saw social institutions as using knowledge as a form of social control.

World War II was a total war that affected every member of society and made everyone’s fitness of interest to the government. Elsie Widdowson (1906–2000) and Robert McCance (1898–1993) became their own experimental subjects and put themselves through various starvation diets, injections and exhausting exercise regimes to help figure out whether wartime rationing would affect people’s health. Widdowson and McCance’s self-tracking led to large-scale state tracking as their work shaped rationing in Britain.
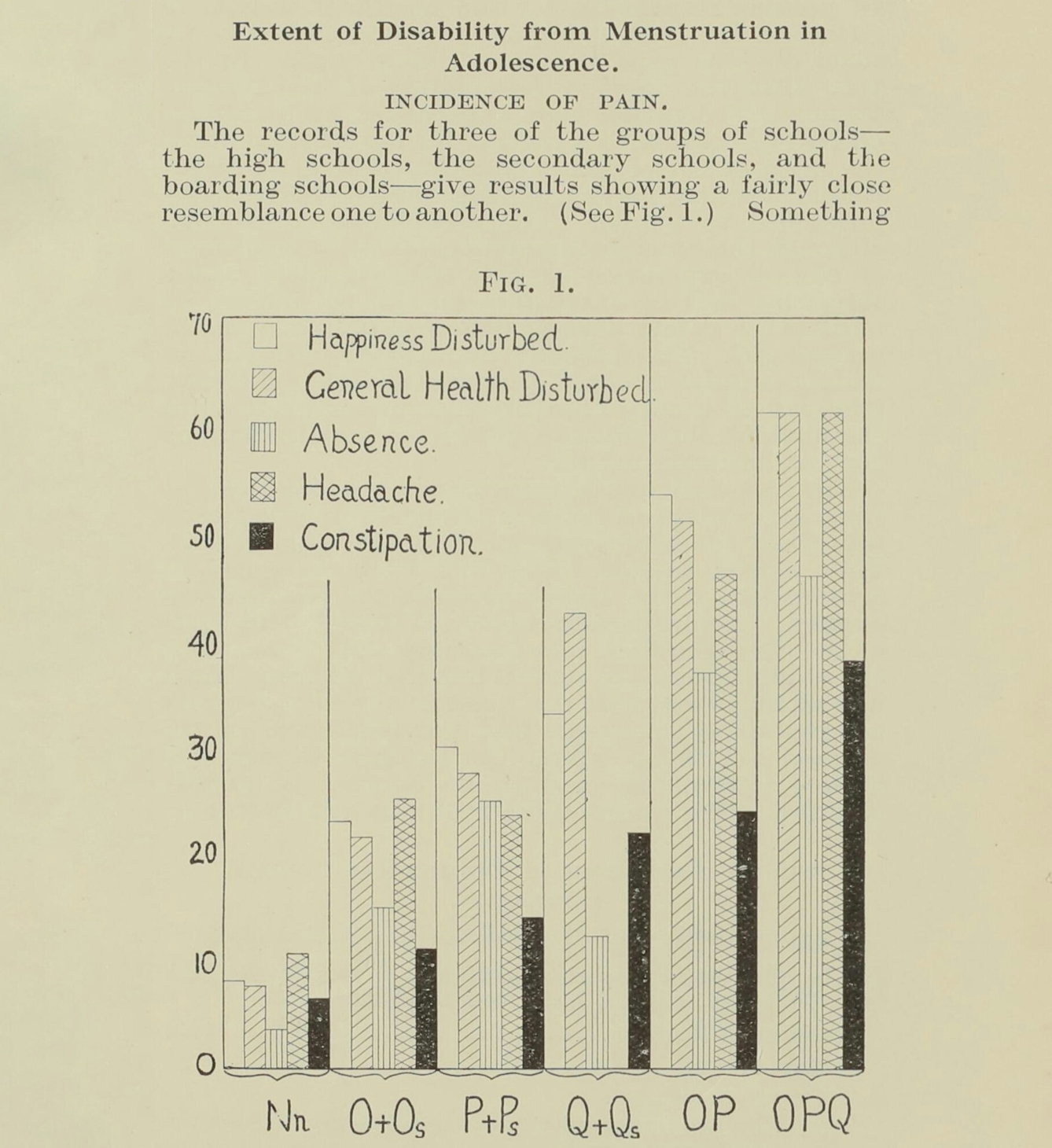
In an earlier project, Widdowson and McCance surveyed female colleagues and acquaintances and collected 220 questionnaires for a study of physical and emotional periodicity in women. Men (and specifically white men) have often been used as the standard measures for health, which can create a dangerous lack of knowledge in women’s healthcare. Women researchers like Widdowson are more likely to develop medical treatments that benefit women. In another example from our collections of women researchers seeking to redress omissions of data on women’s health, the Medical Women’s Federation collected data on schoolgirls’ periods, pregnancy, parenting and employment, and women’s experiences of menopause.

One study of maternity grew to become “the longest continually running major birth cohort study in the world and is one of the longest-running studies of human development” by the Population Investigation Committee. The National Survey of Health and Development began in 1946 through a collaboration with the Royal College of Obstetricians and Gynaecologists. It followed over 5,000 people over the course of their lives and has been used to show the impact of Britain’s National Health Service. It has now developed into a study of ageing. This image is of part of the Survey for 1954 – which is to be filled in by the child’s parents – and shows how health is included with wider societal issues.
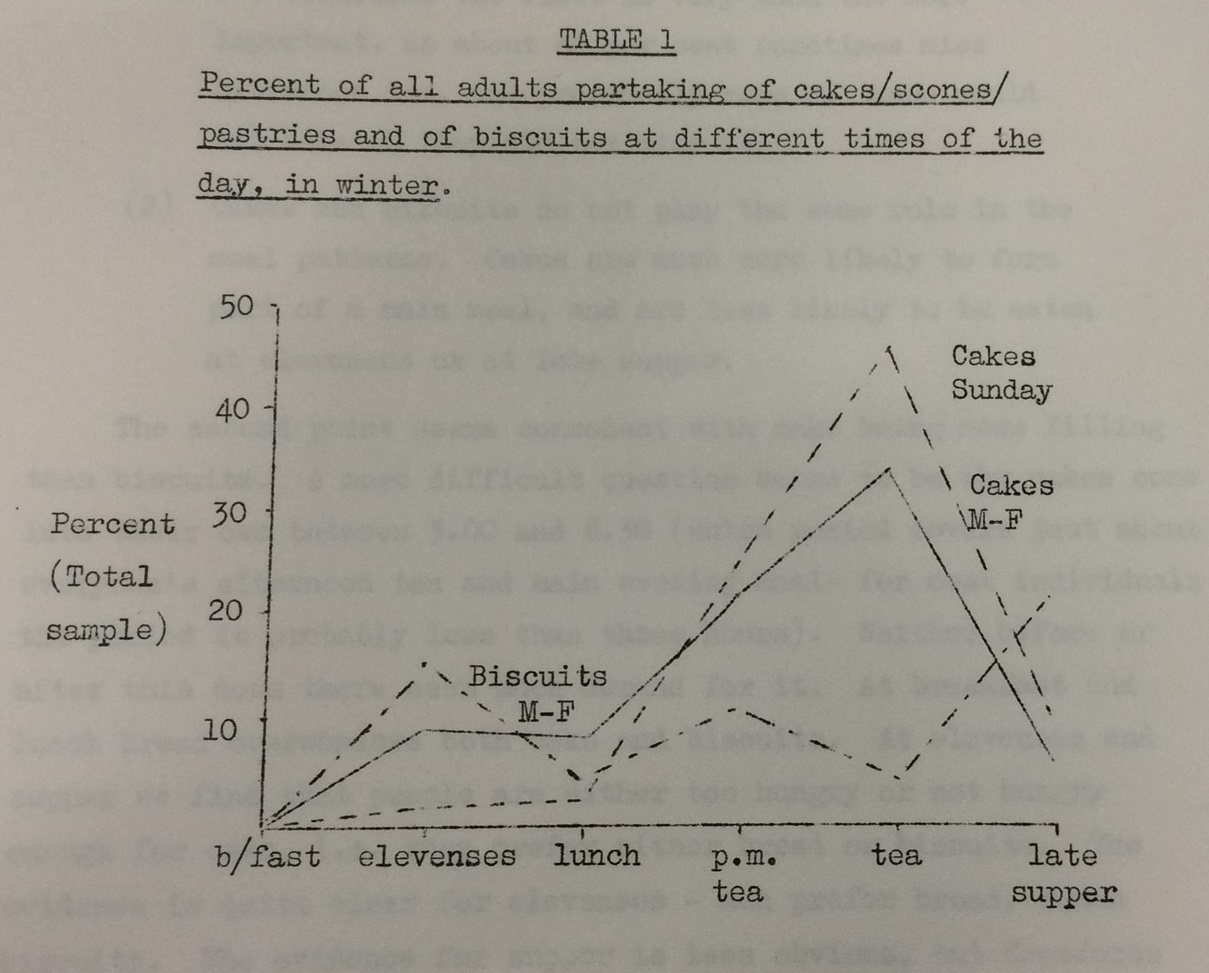
As well as people wanting to know themselves, and governments wanting to know their workers, private companies also want to know their customers. After the war, surveys were increasingly used by businesses and marketing companies in consumer testing. This had crossovers into ideas on health and nutrition. Take, for instance, the graph here, taken from a consumer survey carried out by the Tavistock Institute of Human Relations called ‘Notes on Cake Usage & Preferences'.

After people have been persuaded to buy all that cake, they might be persuaded to lose some weight. This Preludin slide-rule calculator was distributed to medical professionals by the company selling the weight-loss drug Preludin. This calculator could be considered the forerunner to today’s best-known measure today using weight and height, the body mass index (BMI). The BMI was designed by Europeans, using western European data, “as a way of measuring populations, not individuals — and it was designed for the purposes of statistics, not individual health”. Illustrating the dangers of using measures for unintended purposes, BMI detects less than 50 per cent of obesity cases in women.

The objectivity of surveys was reflected upon in ‘Would You Mind?’, a questionnaire designed for the ‘Institute of Sexology’ exhibition which ran at Wellcome Collection from 2014 to 2015. Created by the writer Neil Bartlett, the survey began as a formal survey on the sex life of participants, but then allowed for the participants to suggest a question to be added to the survey. Bartlett chose a different question each week that the survey ran in the exhibition, producing a survey in which the participants also became the surveyors. The completed surveys are now in our collections, offering a disruptive take on the notion of the survey.
We might consider ourselves our own surveyors when we are using one of the 160,000 personalised health and medical apps on the market to track our steps or sleep patterns. However, as the sociologist Deborah Lupton has written: “The data generated from many of these activities are exploited by many different actors and agencies for commercial, managerial, governmental or research purposes.”

Measuring health has different value for different groups. There are dangers of too little data leading to poorer health provision, too much data making us mistrustful, and of data out of our control being used for unintended purposes. As this brief history shows, data gathering has been happening for a very long time and only shows signs of increasing, so perhaps we all need to become more used to pausing and reflecting, “Am I better off for knowing this?”
About the author
Ross MacFarlane
Ross MacFarlane is a research development specialist at Wellcome Collection. He has researched, written and lectured on the collections and other topics at the intersection of death, folklore and medicine.

